Despite thousands of supportive studies spanning more than 40 years showing dietary omega-3 fats EPA and DHA protect against heart disease, the recent publication of a study on the effectiveness of fish oil in heart patients has confused many. One confounding factor was that most of the media sensationalized the story with totally incorrect headlines.
I have called upon longtime omega-3 expert, William Harris, Ph.D., to clarify what research is or is not showing fish oil can do. I have asked Dr. Harris to comment on specific flaws in the Journal of the American Medical Association (JAMA) study and to also discuss the difference between studies of healthy people’s long-term nutrition and the use of a nutrient as if it were an additional pharmaceutical in diseased patients. We will also discuss the two very positive reports in the current American Journal of Clinical Nutrition.
Some of the points that Dr. Harris will discuss are:
1. The meta-analysis was seriously flawed, primarily because it held the fish oil studies to a much higher statistical standard than even drug studies are held.
2. The conclusions were generalized far beyond what the study actually found.
3. The blood levels of EPA and DHA, or the Omega-3 Index, were not determined, so that it cannot be known the extent to which the patients complied with the prescribed amounts of fish or fish oil, or even if patients assigned to the “placebo” treatment started taking fish oil on the side.
4. The effects of EPA and DHA may have been overpowered by strong drugs given at the same t ime.
ime.
Dr. Harris is one of the world’s leading omega-3 researchers. He holds a Ph.D. in nutritional biochemistry from the University of Minnesota and began his omega-3 research in 1979 as a post-doctoral fellow in the laboratory of William Connor, M.D., at the Oregon Health Services University (Portland). Dr. Connor was a leading researcher at the time in nutrition, lipids (fats) and heart disease. Dr. Harris’s early research centered on the possible effects of high quantities of salmon oil on blood cholesterol.
Dr. Harris was the director of the Lipid Research Laboratories at the University of Kansas Medical Center (KUMC) and at the Mid America Heart Institute, both in Kansas City, MO, for 22 years, and was on the faculty at KUMC and at the University of Missouri-Kansas City School of Medicine. Between 2006 and 2011, he was the director of the Cardiovascular Health Research Center at Sanford Research/USD (Sioux Falls, SD).
Over the last 32 years, Dr. Harris’s research has focused primarily on omega-3 fatty acids and cardiovascular disease. He has been the principal investigator on five omega–3-related NIH grants, and is currently evaluating omega-3 blood tests as a possible new risk factor for cardiovascular disease. In 2004, he and his colleague Clemens von Schacky proposed that the Omega-3 Index be considered as a new cardiovascular risk factor, and in 2009 he founded OmegaQuant, LLC to offer the test commercially. In 2011, he became a senior scientist at Health Diagnostic Laboratory, Inc. in Richmond, VA. He retains an academic appointment as professor of medicine at the Sanford School of Medicine, University of South Dakota in Sioux Falls.
Over the years, Dr. Harris has published many major research articles and reviews on the marine lipids, EPA and DHA. A major discovery of Dr. Harris and his colleagues has been the elucidation of the Omega-3 Index as a risk factor in cardiovascular disease. Dr. Harris was kind enough to discuss the Omega-3 Index with us in October 2011.
Dr. Harris’ leadership role in omega-3 research was the reason that the discoverer of fish oil’s role in reducing cardiovascular risk, Jørn Dyerberg, M.D., and I asked Dr. Harris to write the foreword to our recent book, The Missing Wellness Factors: EPA and DHA.
Passwater: First of all, Dr. Harris, Dr. Dyerberg and I wish to thank you for the honor of you writing the foreword to our book. I especially enjoyed your comments about your early research on salmon oil. Would you mind sharing the findings with our readers?
Harris: In the late 1970s, we were unaware of the research of Dr. Dyerberg and Dr. Hans Olaf Bang in Greenland, which pinpointed omega-3 fatty acids as the cardioprotective factors in the Eskimos’ diet. We were simply interested in the overall “polyunsaturated-ness” of fish oil. Would it lower cholesterol like other liquid oils (which were plant- not animal-derived)? Or, would it raise cholesterol like other animal fats (which were solid not liquid)?
We did find that the “liquid-ness” was more important than the “animal-ness” of the oil vis-à-vis blood cholesterol, but when we learned about omega-3 fatty acids from Drs. Dyerberg and Bang, our blinders fell off and we began to see fish oils not simply as liquid animal fats, but as vehicles for incredibly important nutrients—ones that were sadly missing from the American diet.
Passwater: Thanks. Now for our current topic. In September, a flawed report was incorrectly reported by much of the media and has served to confuse many people (1). This report appeared to not agree with the established body of science on fish oil. At about the same time and even since then, additional studies appeared that are supportive of what we have been learning for more than 40 years. Two articles have been published in the American Journal of Clinical Nutrition (AJCN) showing that EPA and DHA are protective against heart disease (2,3). Still another study was published in Brain, Behavior and Immunity that contributed to the body of science showing that EPA and DHA affects the health and longevity of all cells (4).
In the September AJCN, the Nurses’ Health 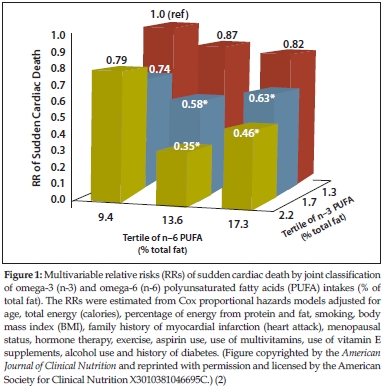 Study group at Harvard published some interesting findings about omega-3 fats and sudden death from heart attacks (2). I find Figure 1 in their report quite interesting. What does the graph tell us? Please interpret it for our readers.
Study group at Harvard published some interesting findings about omega-3 fats and sudden death from heart attacks (2). I find Figure 1 in their report quite interesting. What does the graph tell us? Please interpret it for our readers.
Harris: This figure was taken from a study in which the investigators wanted to know, “Is the kind of fat in the diet associated with the risk of having an acute cardiac arrest (i.e., a heart attack that kills almost immediately unless CPR is administered right away [also called ‘sudden cardiac death’])? They tried to answer this question by looking at data from a large and very prolonged study called the Nurses’ Health Study.
In this study, over 90,000 female nurses were enrolled nationwide over 30 years ago. They were asked to describe their habitual diets; in fact, they were asked to do this every four years (so about eight times) over the period of the study. So, the investigators have a pretty good idea of how much fat and which kind of fat (saturated or land animal fats; or unsaturated, vegetable oils [omega-6] or fish oils [omega-3]) they were eating. Over the study period, more than 300 women experienced sudden cardiac death. So, the question was, “Is there any relationship between which kinds of fats the women typically ate and their risk of sudden cardiac death?”
The graph shows at least one answer to the question. The right axis that goes back into the page plots omega-3 fatty acid intake (written as n-3 in the graph); it includes the fish oil plus the plant omega-3, alpha-linolenic acid (ALA). On the bottom axis is omega-6 fatty acid intake (written as n-6 in the graph). These are each plotted in “tertiles.” That means that the women are categorized into three groups: those who consumed the least (the lowest third), the intermediate (middle third) and the most (upper third) of each kind of fat.
On the vertical axis is the “relative risk for sudden cardiac death.” The top value is 1, which can be considered 100%. If the amount of omega-6 or omega-3 made no difference at all on risk for sudden cardiac death, all the columns would be the same height: all set at 1. If the risk for sudden cardiac death differed according by group, then the columns would be higher than 1 if risk was increased or lower than 1 if risk was reduced.
What we see in the graph is that women who ate the lowest amounts of both the omega fats (the far left position on omega-6 row and the back position on the omega-3 row) had the highest risk of death (so their column is set at 1.0, and is called the ref[erence]). The groups that had the lowest risk (all have asterisks) were those at the intermediate and highest intakes of both the omega-6 and the omega-3 oils, especially the group that reported eating intermediate omega-6 and the highest amount of omega-3 (the 0.35 number means that the risk for sudden cardiac death in that particular group was only 35% of what it was in the reference group). The conclusion drawn from this study is that higher intakes of both the omega-3 (fish and plant) and omega-6 fatty acids help reduce risk for sudden cardiac death… that they are both heart-healthy oils.
Passwater: Looking at this particular group with the lowest risk—the highest intake of omega-3 fats and the intermediate intake of omega-6 fats—does this have any implications for the Omega-3 Index, or is this dietary recall type of study too crude to correlate with an actual blood measurement study? The figure suggests a “U”-shape relationship with omega-6 and omega-3 fats. Can too much omega-6 diminish some of the benefit of omega-3 fats?
Harris: There is no question that having an objectively measured “biomarker” (a blood test) of omega-3 (and omega-6) intakes would have been preferable to using a diet questionnaire in this study. In that regard, using the Omega-3 Index, which is the amount of omega-3 fatty acids in red blood cell membranes and a well-validated test of how much omega-3 people really are eating and absorbing, would have been a more scientific approach. As to whether there really was a “U”-shaped relationship here or not is hard to say. There is no statistical difference between the 35% and 46% columns, and previous studies that have asked similar questions have concluded that both omegas are good for the heart, and neither blocks the actions of the other.
Passwater: The report in the October AJCN also showed that increased fish consumption was associated with decreased heart attack risk (3).
Harris: This is yet another example of a study in which higher fish intake correlates with reduced cardiac risk, and its findings are consistent with the idea that omega-3 fatty acids are protective. We must be cautious, however, in concluding that it was the omega-3 fatty acids in the fish eaten by these people that was responsible for the beneficial effect. In studies like this, it is always possible that either something else in the fish was helpful, or that something that the fish eaters were not eating was harmful, or that there is some other factor at work such that people who eat more fish just live healthier lifestyles. If the researchers had measured the Omega-3 Index in this study and shown that its levels were favorably related to coronary risk, then the conclusion would be a little clearer.
Passwater: In our book, Dr. Dyerberg and I go beyond heart and brain health and discuss how EPA and DHA affect every cell in the body and thus total wellness as well as the prevention of many diseases. The protection of cellular health can be seen by the effect of EPA and DHA on telomeres.
Telomeres are the DNA fragments that protect the ends of chromosomes from deterioration. Telomeres can be likened to aglets, the plastic tips that bind the ends of shoelaces to keep them from fraying.
Telomeres help keep chromosomes intact much like the aglets on shoelaces. As cells replicate over time, the telomeres usually shorten and lose some of their ability to protect the chromosomes. When the telomere becomes too short, the cell is not protected and cannot replicate properly, which leads to impaired cellular health. This process eventually leads to cell death. Dr. Dyerberg and I discuss this in our chapter on longevity and anti-aging where we reported on a study that showed that the higher the Omega-3 Index, the slower the rate of telomere shortening over a five-year period.
Now, a new study has been published in Brain, Behavior and Immunity that asks the question, “Does taking fish oil supplements affect the rate of shortening of telomeres?” (4). What does this study show us regarding the Omega-3 Index and cell aging?
Harris: In this new study from Ohio State University, researchers recruited 106 sedentary adults who were given either a placebo (inactive oil), a low dose (1.25 gm/day) of EPA+DHA or a high dose (2.5 gm/day) of EPA+DHA for four months. Telomere length was measured at the beginning and the end of the study. As the plasma omega-6:omega-3 ratios were reduced (due to the increased intakes of EPA+DHA; not to decreased intakes of n-6 fatty acids), the telomeres not only did not shorten, but they actually increased in length. This could be interpreted as an anti-aging effect of EPA+DHA, consistent with the earlier five-year study.
Passwater: It seems as soon as the book written by Dr. Jørn Dyerberg and myself (which detailed the 40 years of evidence for a cardioprotective effect of the marine lipids EPA and DHA he had discovered) was published, a new study appeared in JAMA that was widely quoted as saying that fish oil was worthless in heart disease. Well, with all this past research and these very recent supportive studies, how could anybody conclude that there is no benefit of fish and fish oils on heart disease?
The JAMA article that I mentioned earlier was a meta-analysis of 20 prior studies on fish oil and cardiovascular disease (1). A meta-analysis is not a new experiment or clinical study, but an “armchair” statistical analysis. The study did not administer any treatment or placebo to the participants; researchers just took already published results, put them into their computer and crunched the numbers. Despite what the TV news may have said, this was not a “landmark” study. A meta-analysis is simply a statistical tool used to group the results from several trials to generate new hypotheses (ideas) to test. This is not a technique to prove an old hypothesis.
Meta-analyses are subject to a number of limitations. The first and most important problem is avoiding bias. Bias is what occurs when a researcher systematically affects the results of his study, consciously or unconsciously, by his inserting his own beliefs or flawed methods.
The meta-analysis showed that an average intake of about 1,000 mg of EPA+DHA for an average of about two years resulted in a 9% reduction in cardiac death, a 13% reduction in sudden death, an 11% reduction in heart attacks, a 5% increase in stroke and a 4% reduction in all-cause mortality. Most of these findings were not “statistically significant,” meaning that we can’t be sure that the observed effects were not just the play of chance.
However, the 9% reduction in cardiac death was statistically significant, and not just at the usual level of 5% (which means that the probability that the effects observed were just chance findings is less than 5%, or a one in 20 chance; this is the standard level of statistical significance used in all medical research). These findings were even stronger with statistical significance at the 1% level (i.e., only one chance in 100 that the reduction in cardiac deaths observed was just due to chance).
However, instead of declaring that their meta-analysis confirmed the cardioprotective effect of omega-3 fatty acids, the authors imposed their own criterion for statistical significance (now it had to be less than one chance in 167 to be declared significant). Since the data did not meet their standard, they (and the news media) concluded that fish oil did not reduce risk for heart disease. What gives with this maneuver?
Harris: The authors justified this on the basis of needing to correct for “multiple testing,” a statistical practice rarely done in meta-analyses. In fact, of the 16 meta-analyses that were published in JAMA during the first nine months of 2012, this paper by Rizos and colleagues was the only one to adjust for multiple testing and the only one not to use the traditional 5% standard to draw their conclusions. Why they changed the rules for this analysis is not clear, but what is clear is that their conclusion was driven by a subjective and controversial interpretation of the data, not by standard statistical practices, that turned a favorable effect of omega-3 into a non-effect.
Passwater: I especially find puzzling how their arbitrary treatment of statistics led them to conclude that there was an increase in strokes. In our chapter on stroke, Dr. Dyerberg and I discussed 16 studies on fish, fish oil and stroke, and found that baked or broiled fish and fish oil supplements were protective against stroke, whereas fried fish was not.
The 2001 Harvard Nurses’ Health Study found that “higher consumption of fish and omega-3 polyunsaturated fatty acids is associated with a reduced risk of thrombotic infarction [i.e., stroke caused by a blood clot], but is not related to risk of hemorrhagic stroke [i.e., stroke caused by bleeding] (5). The next year, Harvard researchers reported similar studies showing reduced stroke risks in men (6). In 2004, a meta-analysis showed that stroke was inversely related to intake of fish with those eating fish five times a week having 18% fewer strokes (7). In 2011, another meta-analysis showed a six to 10% reduction in all types of strokes as fish intake increased (8). The Rizos meta-analysis suggested that fish oil increased the risk of stroke.
Fortunately, a new meta-analysis of 16 previous studies published in October in the European Journal of Clinical Nutrition finds that fish intake markedly reduces stroke risk (9).
Harris: These new data are welcomed of course. The challenge we face is that fish contain much more than just omega-3s, and secondly, that epidemiological studies cannot give us cause-effect relationships, only associations. So, although this new report on fish and stroke is favorable to the omega-3 story, it cannot be considered as reliable as randomized trials with fish oil capsules. Perhaps the largest trial of this nature was a subset of the JELIS trial in which patients with a history of stroke given EPA had a reduced risk of stroke over the next five years. That is strongly supportive of a benefit on stroke.
Passwater: Meta-analyses are supposed to lump very similar studies together. Some of the studies selected used very little fish or fish oil. Is this valid?
Harris: Well, one has to look very carefully at the types of studies included in the meta-analysis because if they are poorly designed, then the conclusions of that meta-analysis will be suspect. Clearly, giving less omega-3 than even current guidelines suggest (which was commonly done in the studies in this meta-analysis) will likely lead to null (“no effect”) findings. In addition, giving small amounts to very ill patients already receiving powerful drugs and procedures for relatively short periods of time is almost guaranteed to have no detectable effects on heart health. A little bit of fish oil will not miraculously cure cancer either.
It would be more meaningful if, for example, only studies in which patients with a low Omega-3 Index and with the same type of heart disease were all given more than 2,000 mg of EPA and DHA for at  least 10 years. That would be a much better test of the question, “Do omega-3 fatty acids reduce the risk for death from cardiovascular disease?” But, such a study has never been done and due to the expense, will probably never be done. So, its results will never be available to lump into a meta-analysis like this one.
least 10 years. That would be a much better test of the question, “Do omega-3 fatty acids reduce the risk for death from cardiovascular disease?” But, such a study has never been done and due to the expense, will probably never be done. So, its results will never be available to lump into a meta-analysis like this one.
Passwater: Dr. Harris, I am sure your explanations will help many of our readers understand the body of science about fish oil, EPA and DHA, and the risks of heart attacks and stroke. Thank you for helping once again. WF
Dr. Richard Passwater is the author of more than 45 books and 500 articles on nutrition. Dr. Passwater has been WholeFoods Magazine’s science editor and author of this column since 1984. More information is available on his Web site, www.drpasswater.com.
References
1. E.C. Rizos, et al., “Association between Omega-3 Fatty Acid Supplementation and Risk of Major Cardiovascular Disease Events: A Systematic Review and Meta-Analysis,” JAMA 308 (10), 1024–1033 (September 12, 2012). doi: 10.1001/2012.jama.11374.
2. S.E. Chiuve, et al., “Dietary Fat Quality and Risk of Sudden Cardiac Death in Women,” Am. J. Clin. Nutr. 96 (3), 498–507 (2012). http://ajcn.nutrition.org/content/96/3/498.abstract.
3. M. Wennberg, et al., “Myocardial Infarction in Relation to Mercury and Fatty Acids from Fish: A Risk-Benefit Analysis Based on Pooled Finnish and Swedish Data in Men,” Am. J. Clin. Nutr. 96 (4), 706-713 (2012); Published online August 15, 2012. doi: 10.3945/ajcn.111.033795.
4. J.K. Kiecolt-Glaser, et al., “Omega-3 Supplementation Lowers Inflammation in Healthy Middle-Aged and Older Adults: A Randomized Controlled Trial,” Brain, Behavior, and Immunity, 26 (6), 988 (2012). doi: 10.1016/j.bbi.2012.05.011.
5. H. Iso, et al., “Intake of Fish and Omega-3 Fatty Acids and Risk of Stroke in Women,” JAMA 285 (3), 304–312 (2001).
6. K. He, et al., “Fish Consumption and Risk of Stroke in Men,” JAMA 288 (24), 3130–3136 (2002).
7. K. He, et al., “Fish Consumption and Incidence of Stroke: A Meta-Analysis of Cohort Studies,” Stroke 35(7):1538-1542 (2004).
8. S. C. Larsson and N. Orsini “Fish Consumption and the Risks of Stroke: A Dose Response Meta-Analysis,” Stroke 42(12):3621-3623 (2011).
9. P. Xun, et al., “Fish Consumption and Risk of Stroke and its Subtypes: Accumulative Evidence from a Meta-Analysis of Prospective Cohort Studies,” Eur. J. Clin. Nutr. 2012 Oct 3. doi: 10.1038/ejcn.2012.133. [Epub ahead of print].
Published in WholeFoods Magazine, December 2012










